Treatments such as IVF may increase risk of hypertension, dysrhythmia and heart failure in the first year after giving birth.
Women who need help falling pregnant may also need more heart-specific help after delivering their bundle of joy.
A new US study, published in the Journal of Internal Medicine, reports patients who undergo infertility treatment are twice as likely to develop cardiovascular disease before their baby’s first birthday.
Infertility treatments and assisted reproductive technologies have previously been associated with adverse outcomes including gestational diabetes and low birth weight. But less has been known about how these treatments and technologies relate to cardiovascular disease, the leading cause of maternal death.
“Postpartum checkups are necessary for all patients, but this study indicates they are particularly important for patients who undergo infertility treatment to achieve a conception,” lead author Dr Rei Yamada told media.
As part of the retrospective population-based cohort study, researchers reviewed 12 months of postpartum medical record data for over 30 million new mothers over nine years. One percent of women used some kind of infertility treatment before conceiving.
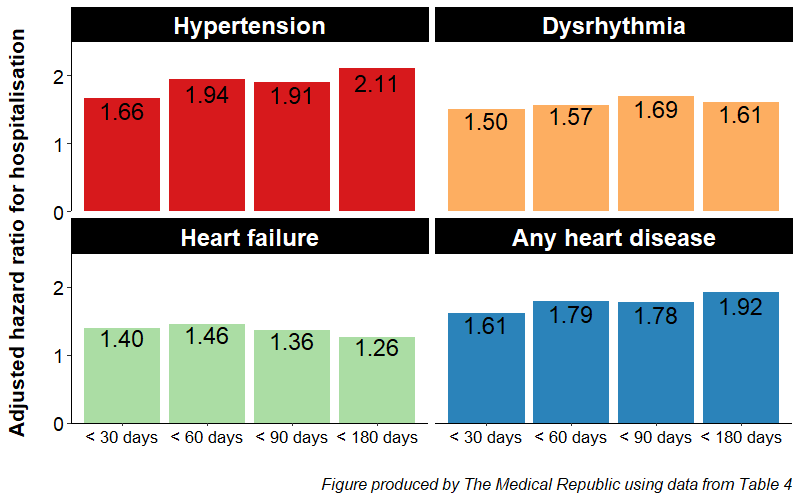
After controlling for factors such as hospital size as well as maternal age and income, patients who underwent infertility treatment were 2.2 times more likely to develop hypertension and 1.75 times more likely to develop a cardiac dysrhythmia in the first year after giving birth.
These associations translate to 195 additional cardiovascular disease-related hospitalisations per 100,000 patients in women who underwent infertility treatment, and 171 additional hospitalisations for hypertension per 100,000 patients.
“This must be taken with the caveat that the overall numbers were small (550 patients versus 355 per 100,000 in the fertility treatment versus conceived spontaneously groups),” said Associate Professor Nikki Bart, a cardiologist from St Vincent’s Hospital and the Victor Chang Cardiac Research Institute in Sydney.
There was no association between infertility treatment and atherosclerosis, cardiomyopathy or heart failure – but patients who underwent infertility treatment were twice as likely to experience any kind of heart disease (a composite measure where any of the six specific cardiovascular diseases occurred).
The increased risk of being hospitalised with cardiovascular disease was present within the first month after giving birth and increased over time. There was also a time-specific association between infertility treatment and heart failure.
Professor Bart told Oncology Republic there were multiple explanations for how infertility treatment could contribute to an increased risk of cardiovascular disease.
“Women who undergo infertility treatment to conceive may be an older age when they become pregnant which places them at a higher risk of hypertensive disorders of pregnancy and pre-eclampsia. They may also already have established risk factors such as hypertension independent of pregnancy.”
The study was limited by the fact patients were only followed for 12 months, with Professor Bart saying a much longer follow-up is likely needed to gain a better understanding of risks associated with the development of cardiovascular disease.
The Australia’s mothers and babies report, produced by the Australian Institute of Health and Welfare, listed cardiovascular disease as the most common cause of maternal death in the decade from 2012 to 2021.
Picking up additional risk factors and offering prevention while women were engaged with the medical system during pregnancy and post-birth is crucial, according to Professor Bart.
“Women have specific risk factors for cardiovascular disease, and women who have gestational diabetes during pregnancy are at risk of heart disease in the future. These risk factors are warning signs for future cardiovascular disease and picking them during pregnancy is an excellent way of managing risk and practising prevention strategies.”